Introduction
Thoracic Outlet Syndrome refers to a collection of symptoms in the shoulder, forearm and hands, which result in pain, numbness, tingling and weakness in the arm or hand.
The symptoms result from the compression of arteries, nerves and/or veins which pass through a narrow area at the front of the lower neck referred to as the ‘thoracic outlet’.
The thoracic outlet is a confined space between the first rib and the collarbone (clavicle) through which important structures, including the subclavian artery, vein, and nerves (the brachial plexus: a complex network of nerves from the neck region) pass through. It is this congested anatomy that increases the potential for this syndrome.
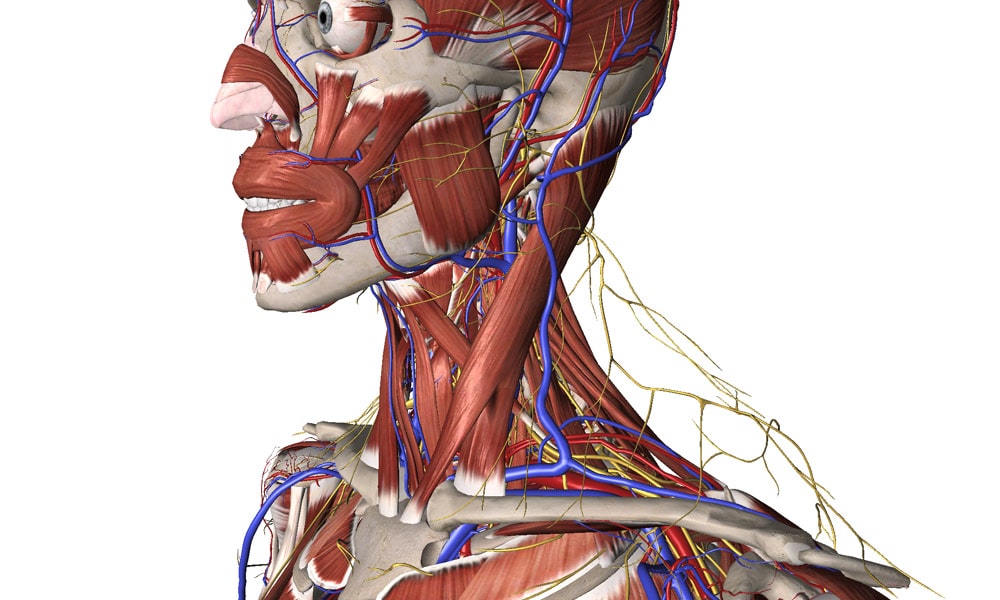
Types of Thoracic Outlet Syndrome
There are a number of ways that thoracic outlet syndrome can present, each depending on the affected structures.
Thoracic outlet syndrome can be:
Neurogenic – this accounts for over 90% of cases, and affects the nerves from the cervical region of the spine (which control movements of the shoulder, arm and hand). Neurogenic thoracic outlet syndrome results numbness, pain, and sometimes even weakness in the arm muscles.
Venous – this is the second most common cause of thoracic outlet syndrome and accounts for approximately 10% of cases. It is caused by mechanical compression and irritation of the subclavian and axillary veins between the clavicle and the first rib. This can reduce or obstruct blood flow in this region, potentially causing a clot; this is a medical emergency.
Arterial – this is the least common form of thoracic outlet syndrome and accounts for approximately 5% of cases. It is often a result of the subclavian artery becoming compressed within the scalene triangle (between the anterior, posterior and medius scalene muscles). It can also develop into a medical emergency, so careful examination is vital.
Signs and Symptoms of Thoracic Outlet Syndrome
- Numbness and/or tingling in the affected arm
- Cold hands and a pale blue discoloration of the fingertips
- Pain and swelling in the neck, arm, and hand
- Weakness in the of muscles of the involved limb
- Absent or weak pulse in the arm (as felt by a clinician or therapist)
Causes of Thoracic Outlet Syndrome
Thoracic outlet syndrome can have several causes, including:
Poor posture – drooping or rounded shoulders along with protracted scapula (shoulder blade). This narrows the area of the thoracic outlet making compression more likely.
Congenital anatomical abnormalities – cervical rib (extra rib in the neck) and anatomical variations in the neck bone structures.
Trauma – an injury resulting from a traumatic event such as sternum fracture.
Serious – cancers in the arm and upper chest can put pressure on the region.
Diagnosis and Tests
A careful history and examination is extremely important because there are many conditions that mimic thoracic outlet syndrome.
Clinical examination includes the Adson’s test and Roos test, the latter is the one that is most widely used for diagnosing thoracic outlet syndrome.
Tests are guided by the findings of the physical examination and the type of thoracic outlet syndrome suspected is led by the presenting symptoms.
Imaging tests include X-rays of the neck and chest to rule out cervical spine abnormalities, and looking for the presence of a cervical rib (extra neck rib).
Other tests include nerve conduction tests or even vascular studies to detect any abnormalities present in the blood vessels. Occasionally, CT or MRI scans may also be requested by clinicians in more complex cases.
Thoracic Outlet Syndrome Treatment
Treatment aims to decrease symptoms and manage pain. The options vary according to the type of thoracic outlet syndrome presenting.
A doctor or therapist will discuss the most appropriate treatment which can often be as simple as tailored manual therapy.
Neurogenic Thoracic Outlet Syndrome (Physical Therapy)
Osteopathy – osteopathic treatments aim to relieve muscle tension, increase mobility, range of motion, and improve stiffness in the neck and upper limb region. The patient is educated on specific postural adjustments and stretches.
Soft tissue mobilisation (STM) – this is a technique in which light pressure is applied and stretching movements of the muscles and tendons are performed. This reduces the pressure on the structures in the thoracic outlet.
Deep tissue massage – this treatment targets the deep muscles of the neck and arm and is more invasive than mobilisation. This technique involves applying sustained pressure on certain muscle trigger points including the scalene muscles. The Scalene muscles are three muscles which are connected to the neck and rib. They are prone to becoming ‘tight’ with everyday posture such as rounded shoulders from driving or sitting a desk for prolonged periods of time. This helps reduces muscle tension, break any myofascial adhesions, improves blood flow, and helps decompresses nerves and vessels.
Chiropractic treatments – such treatments typically involve the manipulation of the cervical spine and upper ribs to allow a ‘release’ of any structures which may be in ‘locked’ or in spasm.
Note to Patients:
Soft tissue interventions should only be performed by qualified sports massage therapists that hold advanced sports massage qualifications, like the Level 4 Sports Massage Therapy qualification for example. Most level 3 sports massage therapists are unlikely to have sufficient knowledge or experience of this condition.
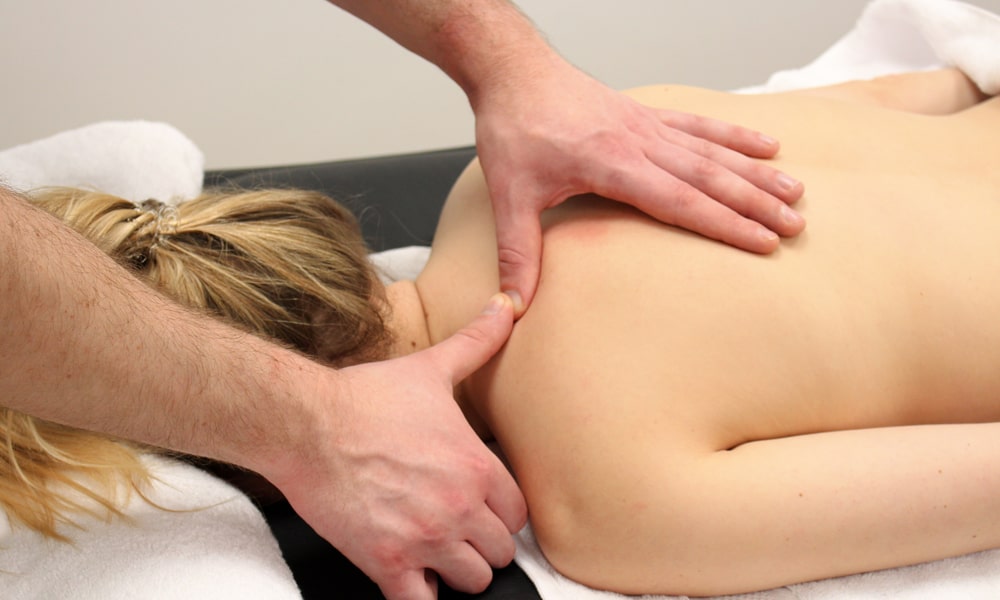
Soft Tissue Mobilisation
Neck (cervical) muscles which are affected by thoracic outlet syndrome can be effectively treated via soft tissue mobilisation. This is often a therapy performed by osteopaths and suitably trained and qualified sports massage therapists.
Gentle mobilisation of the sternocleidomastoid and scalene muscles, along with the pectoralis major and minor muscles, can help to open out the thoracic outlet. Often, the shoulder area is also treated, particularly the rotator cuff, to help with shoulder movement and posture, and to ease the protraction of the scapula which may be contributing to the problem
Deep Tissue Massage of Cervical Muscles
Cervical muscles are massaged with pressure, especially the scalene muscles because they are at a high risk of being affected by thoracic outlet syndrome. Deep tissue massage to both the pectoralis minor attachment on the coracoid process and the deeper scalene muscles is very effective, and results can be realised relatively quickly with patients reporting an easing of symptoms.
Conclusion
Thoracic outlet syndrome can be a debilitating condition, but thankfully it is treatable if caught early and treatment is performed by a competent clinician or therapist. Consulting with a clinician as soon as possible is crucial to preventing long term and potentially more serious complications of the condition. If the condition is allowed to progress, it may become chronic and much more complex.
